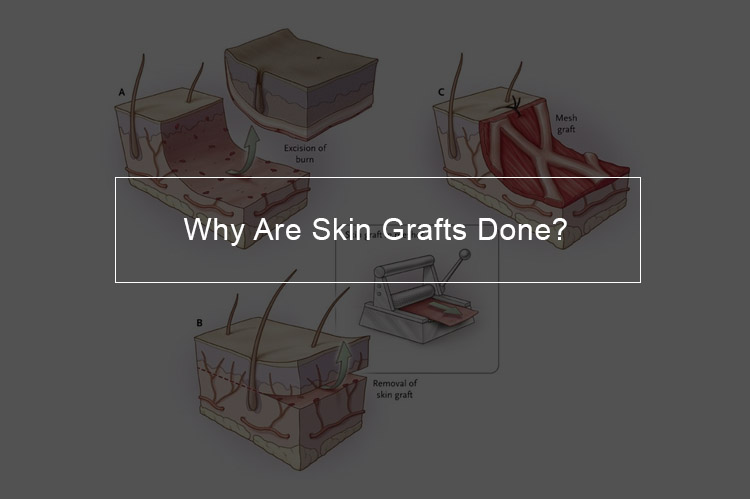
Skin grafting is a surgery involving separating and transferring or reattaching skin from a region of the body to another region of your body. This surgical process can be performed if a portion of the human body has dropped its safety skin cover owing to injury, burns, or disease. Skin grafts are surgeries done within a hospital. Majority of skin grafts are performed with sedation, which implies that during the operation you will be unconscious and feel no pain. A skin graft is placed over an area of the body where the skin has been lost. Skin grafts are done due to include: severe burns, skin contamination, large, open wounds, bedsores and other skin ulcers which have not healed properly and surgery of skin cancer.
Where Does the Skin Graft Come From?
Donor Site For Skin Grafts
Generally, the most effective skin grafts are those using the individual's own skin. It is collected from some other body region and is referred to as an autograph. Once extracted from an identical individual twin, skin grafts could also be effective. There is a greater possibility that the body will reject the fresh skin when a distinct individual is not an identical twin. The body considers it as a foreign intruder organism and fights it through the immune response.
Despite the donor skin being rejected, the graft can be effective by providing plenty of time and safety to the body of a patient to develop fresh skin alone. Alternate methods of graft are intended for momentary use only until the individual's own skin regrows. These options involve: skin removed from a corpse (known as an Allograft) skin removed from an animal (known as a Xenograft) synthetic tissue With such graft or an autograft taken from a twin, your doctor will take care anytime necessary to collect the donor skin from a portion of the body usually covered by clothing. Surgeons will also attempt to match skin texture and color between the donor and the beneficiary as accurately as possible. The most popular donor regions are the buttocks and inner thighs. It is also practicable to choose the forearm, upper arm, abdomen, and back.
Types of Skin Grafts
What are the Three Types of Grafts?
Three basic categories of grafts are available: full-thickness, split-thickness, and composite grafts.
What is a Split-thickness Graft?
A split-thickness graft means removing the epidermis which is your skin's top layer— but also a part of your skin's deeper layer, known as the dermis. The donor site of these layers are the location of healthy skin. Generally, split-thick skin grafts are collected from the outer or front thigh, buttocks, abdomen, or back.
Large regions are covered by split-thickness grafts. These grafts are likely to be brittle and generally look bright or smooth. Skin grafts may also look darker than the skin adjacent to them. Split-thickness grafts do not develop as easily in comparison to ungrafted skin, so as they grow older, kids that get them might need extra grafts.
What is Full-thickness Graft?
This type of grafts includes removing from the donor region all the dermis and epidermis. These are generally areas above the collarbone, groin, abdomen, neck, or region. They're likely to be lower parts of the skin because in a straight-line surgery with staples or stitches the donor region from where it is collected is generally pulled together as well closed.
Usually, full-thickness grafts are used on extremely visible areas of the body, such as your face, for tiny injuries. Full-thickness grafts differ from split-thickness grafts in that they blend well with the surrounding skin and tend to result in a better beauty result.
What Is a Composite Graft Made of?
This graft may cause cartilage, skin, fat, and muscle to be removed. Generally, these grafts are utilized in fields like the nose that needs three-dimensional restructuring. Due to its complicated three-dimensional framework, nasal ala faults are difficult to reconstitute. Effective reconstruction of these faults requires cosmetic symmetry and nasal function preservation. Nasal ala faults have been outlined in a broad range of reconstructive alternatives, varying from locoregional flaps to skin grafts, and also involve the auricular composite graft. When the nasal ala condition is restricted to your skin and the (LLCs) lower lateral cartilage remains intact, restoration can take place without consideration to provide the ala with supporting structure. Additionally, the same concepts for the restoration of the skin layer must still be implemented for these restoration algorithms for deeper flaws affecting nasal and cartilage lining.
How to Prepare for a Skin Graft?
Pre-care Procedure for Skin Graft Surgery
The surgeon will probably book your skin graft appointment a couple of weeks in time, to have time to prepare for the operation. Inform a surgeon in advance about any medicines you are taking on the doctor's recommendation or over-the-counter (OTC). Some medications may compromise with the capacity of your blood to clot, like aspirin. A surgeon may ask you to adjust your prescribed dose until the surgical procedure or to quit taking these medicines. Smoking and tobacco substances will also affect your capacity to cure a skin transplant, so the doctor will probably ask you to quit smoking before the surgery.
The surgeon will also let you know after midnight during the day of operation to consume nothing. If you are nauseated by anesthesia, this is to avoid you from choking and vomiting at the time of operation. You must also intend to bring along a friend or family member following the surgery to drive you back. Local anesthesia following the operation, you may develop drowsiness, so you should avoid driving until the impacts are completely worn off. Having someone remain with you for a couple of days following the end of the operation is also an effective idea. You might need assistance to accomplish certain duties and mobility in your house.
How Long Does a Skin Graft Procedure Take?
Skin Graft Procedure
A bandage which will protect the injury without binding to it will as well cover the donor region.
How a Skin Graft Is Done: There's wound preparation before the operation. Cleaning and measuring the wound. A mechanism for transferring to the donor region can then be traced. You'll be given a local Anesthesia. The operation may involve local, general, regional anesthesia, iv sedation, or a mixture of these options, based on the size, seriousness, and place of the injury, as well as the form of graft. The skin of the donor is collected and ready. A doctor will start the surgery by transferring skin from the donor area.
A surgeon will start the surgery by taking the skin out of the donor region. If you get a split-thickness type of graft, the hair will be separated from a region of your body generally concealed by garments like the outside of your arm or hip. If you get a full-thickness graft, groin, abdomen, or neck region above the collarbone are the desired donor regions. As soon as the doctor removes the skin from the donor region, it will be closely placed over the transplant region by the surgeon and secured with surgical dressing, stitches or staples. It could be "meshed" if this is a split-thickness graft.
The surgeon may punch various openings in the graft to extend the piece of skin to allow less skin from your donor region to be harvested. This also makes it possible to siphon fluid from underneath the graft. Underneath the skin graft, there can be fluid collection that can lead it to fail. In the longer run, meshing can trigger a "fish-net" shape of the skin graft. Thus the donor region is closed.
This is accomplished with incisions with a composite or full-thickness graft. There is no need for incisions at the donor regions with a split-thickness graft. The shell is put on the site of the recipient. After placing the shell in place, the skin graft is attached with incisions or staples to the neighboring tissues. A pressure dressing is placed across the site of the receiver of the skin graft. For the initial 3 days, a unique vacuum device known as a wound VAC can be put over the region to regulate drainage and boost the likelihood of survival of the skin graft.
Recovery starts. Initially, at the beneficiary region, the skin graft utilizes nourishment from the tissue to sustain. During the initial 36 hours, fresh blood vessels start to develop, followed by fresh skin cells that start to develop from the skin graft to envelop the recipient region with fresh skin.
Postoperative Care: It is important to keep both the recipient and donor regions moist and well protected. Your doctor will advise you to use medicines and dressing properly.
Aftercare for a Graft
Skin Graft Surgery Post Care Guidelines
Following a surgery completion, the hospital workers will observe you carefully, track your vitals and give you pain management medicines. If you have had a split-thickness transplant, the surgeon would like you to remain in the hospital for a couple of days to ensure that the transplant and donor region heal properly.
Will My Body Take the Skin Graft?
The skin graft ought to begin to develop blood vessels inside 36 hrs and interact with the neighboring skin. In case the blood vessels do not start to develop soon after the operation, it might be an indication that the skin graft is rejected by the body.
Doctor's suggest a number of reasons for the body not taking a graft such as infection, fluid-like blood gathering underneath the graft, or excessive graft motion on your wound. If your blood circulation to the grafted region is poor or you smoke, your body will likely reject the graft. If your body rejects the initial graft you will likely need a fresh graft or new surgery.
What to Expect at Home After Graft Operation?
Your physician will prescribe painkillers for you when you return home from the surgery to assist in minimizing pain. They will also teach you how to take care of the site of the skin graft and the donor region so that they are not infected. After about a week or two, the donor region will heal, however, the graft site may take a little longer to cure. You will need to prevent doing any operations that might strain or harm the graft region for a minimum of 3 weeks following the procedure. The surgeon will inform you when you're ready to get back to your everyday operations.
How Do You Care for Skin Grafts?
Care of the Healed Graft and Donor Site
You will be told to massage and moisturize the skin graft and donor region using a non-fragrance sorbolene cream about 3 times each day after the region is cured. The reason for this procedure is during the injury, your sweat glands were damaged and you'll need to frequently replace the region with moisture, or else the site may decompose and more scarring may happen.
For a minimum of a year following the surgery, it is essential that you safeguard both regions from the ultraviolet rays. Don't forget to use a sunscreen with minimum SPF of 30, sun protection attire and a cap if you step outside.
If you require a skin graft because of a skin burn, you will consult an Occupational Therapist to discuss scar handling alternatives like the usage of topical silicone items and pressure clothing. They are also going to clarify and promote you to proceed with massage and moisturizer. It is essential that you stick to the Occupational Therapist's guidelines on how to use these products and ways of caring for them.
Risks & Complications of Skin Grafts
Symptoms of Skin Grafts Fails
Skin grafting risks and possible problems are:
- Infection
- Bleeding
- Rejection or death of the skin graft
- Hematoma
- Unsuitable aesthetic results, like scarring, skin texture discoloration or irregularities
- Risks of anesthesia
- Reduction or loss in skin sensitivity
- Heightened sensitivity; rare cases of chronic pain




